 Today, my friend Andrea McDaniel, Holistic and Integrative Registered Dietitian, is going to teach you about a little hormone called leptin. Meanwhile, I am busy in the kitchen creating healthy low-carb recipes for the collaborative cookbook project I am working on, due out in December. ♥ Vanessa
Today, my friend Andrea McDaniel, Holistic and Integrative Registered Dietitian, is going to teach you about a little hormone called leptin. Meanwhile, I am busy in the kitchen creating healthy low-carb recipes for the collaborative cookbook project I am working on, due out in December. ♥ Vanessa
A Lesson on Leptin
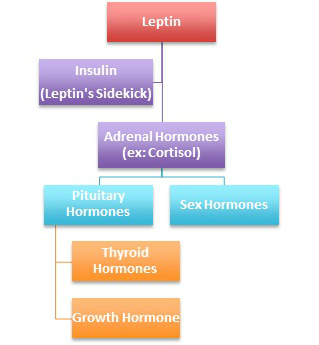 Leptin is considered to be the master hormone, in control of all other hormones. Nora Gedgaudas, well renowned certified nutritional therapist, explains leptin as being on top of “an intricate hierarchical system of management.(1)” As you can see from the simplified graphic to the right, leptin sits at the top as the master controller of all of the other hormones that affect not only our weight but our overall health.
Leptin is considered to be the master hormone, in control of all other hormones. Nora Gedgaudas, well renowned certified nutritional therapist, explains leptin as being on top of “an intricate hierarchical system of management.(1)” As you can see from the simplified graphic to the right, leptin sits at the top as the master controller of all of the other hormones that affect not only our weight but our overall health.
The New Kid on the Block
Leptin was only recently discovered in 1994. According to Dr. Ron Rosedale, nutritional and medical expert at the forefront of leptin research, leptin is still so new that most doctors may not have heard of it nor know what it does, but the more and more scientists research it, the more they are finding out about how vital it is to life.(2)
I can remember the first time I heard about leptin, I was in my first graduate level class. My professor, Dr. Michael Burlock, who does research on the mechanisms that underlie obesity and inflammation, was excitedly explaining to us about the recent discovery of leptin. In his research, he was mostly focusing on insulin (which is still a part of it all), but he had begun to shift to look more into leptin. He and others thought it may be the “missing link” to the complex, but prevalent issue of obesity.
Where is it Found
Leptin is found primarily in the fat cells. Before the discovery of leptin, fat used to be thought of as just excess mass. Researchers now know fat is actually an active organ that produces leptin and other hormones as well as inflammatory molecules.
How Does it Work
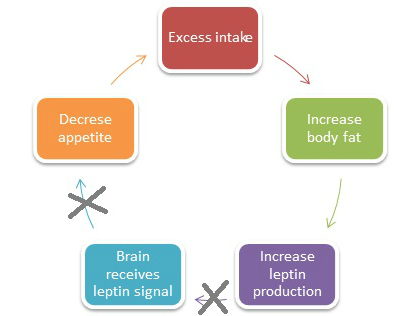
When everything is functioning optimally, adipose tissue or body fat stores produce and release leptin, which tells the brain the body is fed and energy stores are adequate. In turn, our appetite is suppressed and our food intake decreases. If leptin does its job, we would always get a signal to stop eating when we have enough energy in storage.
 When it Goes Wrong
When it Goes Wrong
The problem is not leptin per se, it is leptin resistance. With leptin resistance, the brain stops listening to the leptin signal. It’s like a nagging child. You may hear the nags in beginning, but after a while you become tolerant to the noise, and it no longer has the same annoying effect on you. The same goes for leptin. The brain becomes tolerant or resistant to the cries of leptin.If leptin is no longer being heard by the brain, we don’t benefit from its positive effects of a decrease in appetite and increase in body fat being used for fuel. In turn, the body fat cells continue to produce more and more leptin, creating a viscous cycle.
What Causes Leptin Resistance
Before I tell you how to stop this cycle, we need to know what causes it. The main cause is blood sugar surges caused by excess carbohydrate intake, especially refined, processed carbohydrates that breakdown into sugar quickly. You may be thinking, this sounds like the same main cause of insulin resistance. You’re right. In fact, Nora Gedgaudas describes leptin and insulin as “two birds of a feather.” What disrupts one disrupts the other. Insulin resistance usually comes after leptin resistance, so the earlier you can turn it around the better, but it’s never too late.
Signs and Symptoms of Leptin Resistance
- Overweight
- Fatigue after meals
- “Love handles”
- Increased blood pressure
- Crave “comfort foods”
- Easily anxious or stressed out
- Hungry all the time or at odd hours, like at night
- Osteoporosis
- Difficulty losing weight or keeping it off
- Sugar cravings
- Stimulant-reliance
- Increase in triglycerides
- Urge to snack after meals
- Trouble falling or staying asleep
- Body stays the same no matter how much you exercise
Learn to Listen to Leptin
- Lower carbohydrate intake. Remember the brain is tired of leptin, so we need to give it a break from the loud leptin surge that follows excess carbohydrate intake. You can do this by keeping your carbohydrate sources limited to vegetables.
- Adequate intake of protein. Aim for one or more servings of protein at each meal. A serving is approximately the size of one deck of cards
- Moderate to high healthy fat. So, if we decrease carbs, and keep protein adequate, what’s left? Fat! Yes, I said it. Healthy fat should make up the majority of your calories. Healthy fat includes: fish oil, organic butter, ghee, coconut, avocado, olive oil and olives, fat from animal meat and eggs, and some nuts and seeds.
- Manage stress levels. Diet is not the only thing that impacts blood sugar levels, so does stress.
- Avoid “stressful” foods. This includes grains, vegetable and hydrogenated oils, high fructose corn syrup, processed dairy, soy, corn, and any other foods you may be intolerant to. We aren’t made to eat many of the processed foods found in the supermarket today. The body has to work hard to digest these foods, making modern diet an often overlooked source of stress.
- Sleep. Ideally you need about 8 hours of sleep per night. Sleep plays an important role in regulating leptin levels and in controlling appetite.(3) During sleep, leptin levels naturally rise. If you don’t get enough sleep, low leptin levels will cause an increase in appetite, especially for high-carbohydrate foods.
Conclusion
As you can see, leptin is an extremely important hormone. In order to keep the brain and body happy, it is important to eat a diet and live a lifestyle that promotes optimal leptin levels. I recommend fully committing to at least 3 weeks of implementing the recommendations above. Training the body to listen to leptin and burn fat instead of carbohydrates does not happen overnight and there is no pill that will do this for you. Over time you will notice a sense of freedom from the stronghold that increased appetite and cravings may be having on you, your waistline and your health.
References
- Gedgaudas, Nora. (2011). Primal Body, Primal Mind: Beyond the Paleo Diet for Total Health and Longer Life. Rochester: Healing Arts Press.
- Rosedale, Ron & Colman, Carol. (2004). The Rosedale Diet. New York: Harper Collins Publishers.
- Van Cauter, E. The Journal of Clinical Endocrinology & Metabolism, November 2004; vol 89: pp 5762-5771.
About Andrea
 Andrea McDaniel, is a Registered Dietitian, Sports Nutritionist, Certified Personal Trainer and owner of My True Health, LLC. Andrea believes in an integrated approach to achieving true health and weight loss. She helps her clients get off the disease path and onto the path towards optimal health by getting to the root cause of their health issues.
Andrea McDaniel, is a Registered Dietitian, Sports Nutritionist, Certified Personal Trainer and owner of My True Health, LLC. Andrea believes in an integrated approach to achieving true health and weight loss. She helps her clients get off the disease path and onto the path towards optimal health by getting to the root cause of their health issues.
Copyright © 2012 Andrea McDaniel, My True Health, LLC
This article is not intended for the treatment or prevention of disease, nor as a substitute for medical treatment, nor as an alternative to medical advice. Use of recommendations in this and other articles is at the choice and risk of the reader.
Like Andrea on Facebook
Follow Andrea on Twitter
Visit Andrea at My True Health, LLC